The Entropic Gut: A Three-Part Inquiry into Functional Stability
In the quiet, often internal theater of the human body, few conditions are as capricious as Irritable Bowel Syndrome. Patients frequently describe the condition as a puzzle with missing pieces, a state where a food tolerated one day becomes a source of profound distress the next. This functional disruption occurs within the enteric nervous system and the microbiome, existing in a state of persistent dysregulation. It is essential to distinguish this functional instability from Inflammatory Bowel Disease (IBD). While IBD presents with structural ulceration and measurable immune-mediated tissue damage, IBS is defined by hypersensitivity and signaling errors in a physically intact tract (Gastroenterology). To address this volatility, a contemporary three-pillar framework suggests a method to stabilize motility and recalibrate the gut-brain axis.
The Dietary Calculus of Fermentation
The primary intervention for symptomatic relief begins with the identification of provocative dietary inputs. Wheat is frequently cited as a primary offender, not merely due to gluten but because of amylase-trypsin inhibitors (ATIs) and fructans. These compounds are classified as fermentable oligosaccharides, disaccharides, monosaccharides, and polyols (FODMAPs). They are poorly absorbed in the small intestine and become fuel for colonic bacteria, leading to the osmotic shifts and gas production that define the IBS experience (Nutrients). Identifying these variables is essential, as discussed in Identifying Your IBS Triggers.
The therapeutic objective involves a strategic shift toward soluble fiber. Unlike insoluble fiber, which can act as a mechanical irritant to a hypersensitive gut, soluble fiber absorbs water to form a viscous gel. This process smooths the transit of stool and provides a gentle substrate for bacterial fermentation, as explored in The Science of Soluble Fiber.
Clinical food recommendations for stabilizing the gut include:
Steel-cut oats, mashed sweet potatoes, and peeled zucchini.
Husked and well-cooked chickpeas or hummus in moderate portions.
The avoidance of high-fructan aromatics such as onions and garlic.
The limitation of stone fruits including apples, pears, and peaches.
The removal of alcohol and high-lactose dairy to reduce intestinal irritation.
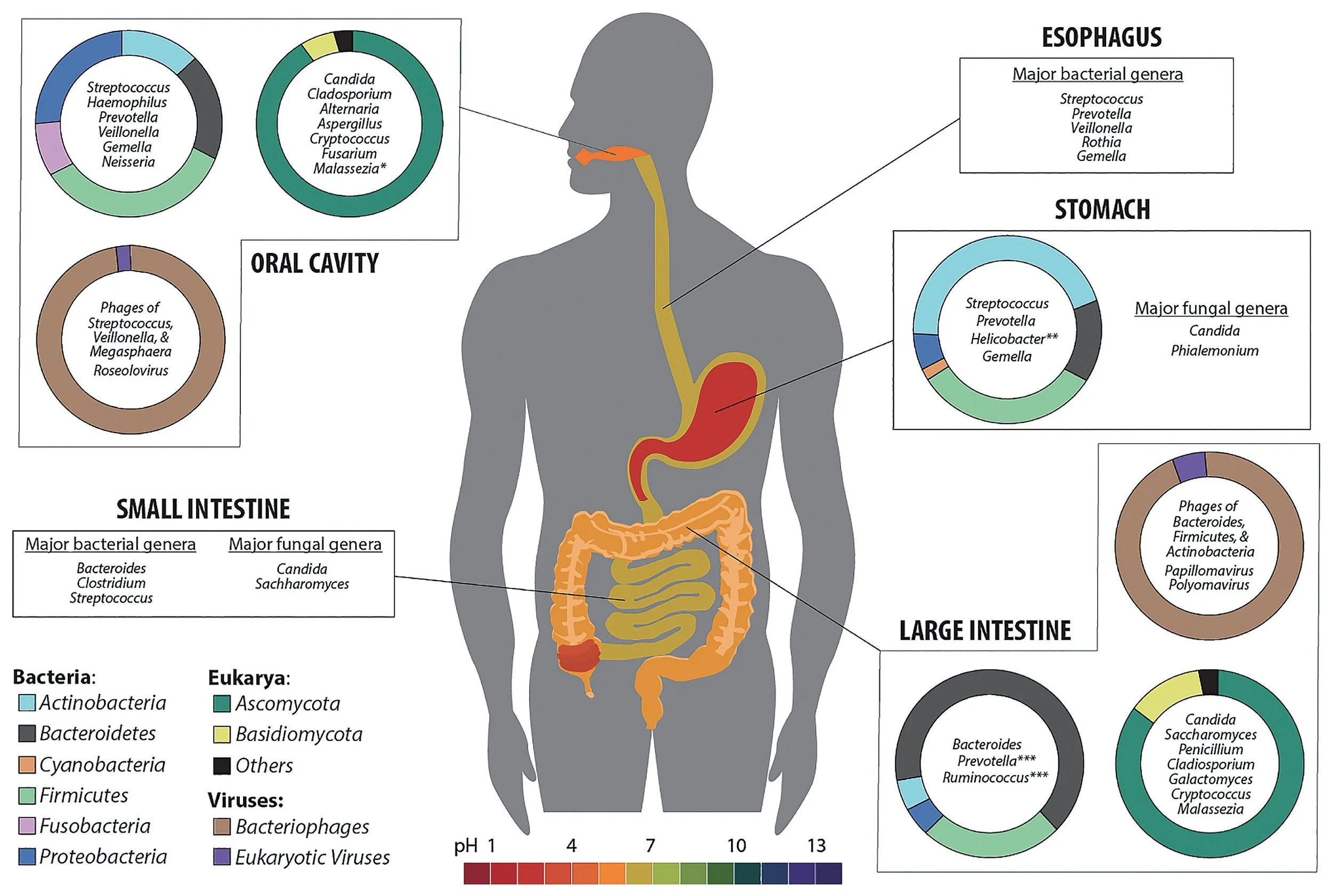
Diagram of human gut microbiome depicted in various regions. Source: Wikimedia
Microbiotic Restoration and the Probiotic Signal
The second pillar involves the modulation of the gut microbiome through daily broad-spectrum probiotics. In patients with IBS, the microbial landscape is often characterized by dysbiosis, a reduction in diversity that correlates with increased visceral hypersensitivity (Nature Reviews Gastroenterology & Hepatology). The introduction of specific strains, particularly those from the Lactobacillus and Bifidobacterium genera, is associated with a reduction in gas-producing bacteria and an improvement in the mucosal barrier.
The efficacy of such interventions is rarely immediate. Clinical observation suggests that a period of two to four weeks of consistent administration is required to achieve a measurable shift in the microbial environment. Spore-based probiotics are also increasingly recognized for their resilience. These organisms are better able to survive the acidic conditions of the stomach before colonizing the large intestine (NIH).
Cannabigerol and the Enteric Nervous System
The most modern addition to this framework is the use of Cannabigerol (CBG), a non-psychotropic cannabinoid. The molecular formula of CBG, C21H32, represents a compound with a high affinity for receptors integrated into the gut-brain axis. Research suggests that CBG interacts with Alpha2-adrenoceptors and PPAR-gamma receptors, which are instrumental in modulating gut motility and visceral pain (British Journal of Pharmacology).
By addressing the overreactivity of the enteric nervous system, CBG may reduce the intensity of peristaltic spasms. This calming effect is a critical component of the multimodal approach, as detailed in The Gut-Brain Connection and CBG. Patients frequently report improved baseline calm when CBG is integrated into a morning or pre-meal regimen to minimize post-meal symptoms.
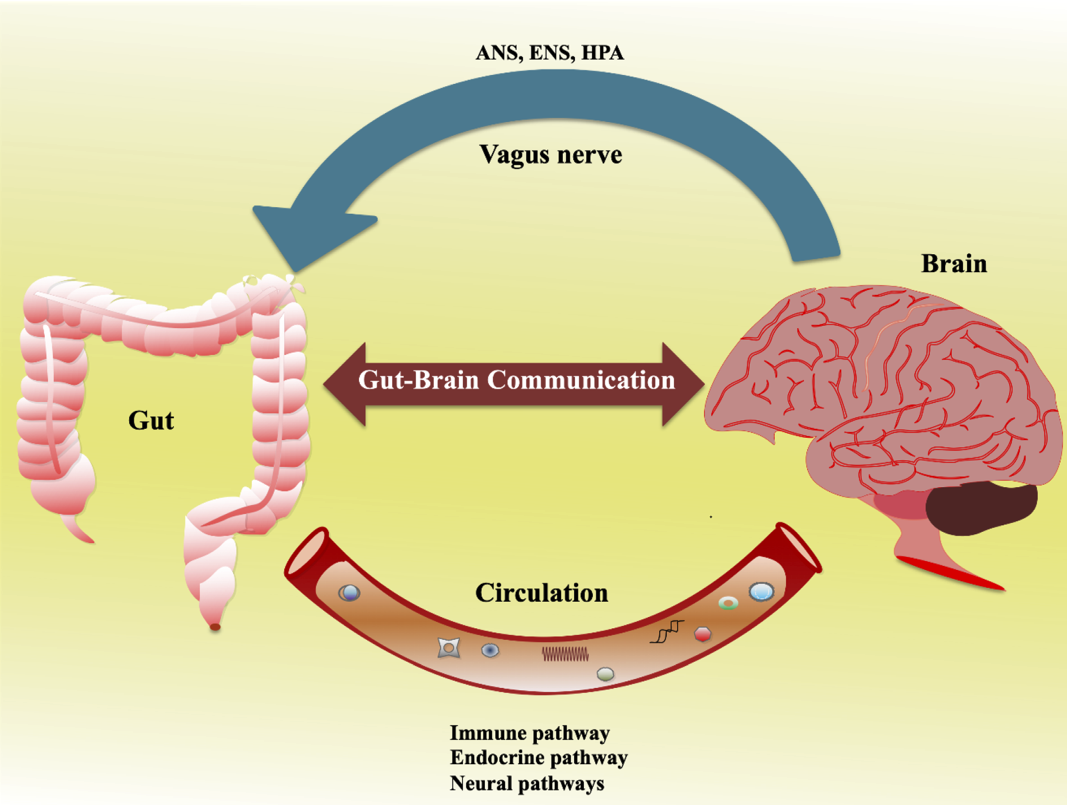
Schematic diagram showing the communication between the gut and brain. Source: Wikimedia.
The Synthesis of Stability
When these three pillars are combined, they create a synergistic effect that addresses the multifaceted nature of IBS. Diet removes the provocative inputs, probiotics rebuild the microbial foundation, and CBG provides a layer of neurological calm. Over a trajectory of two to six weeks, this integrated system facilitates a transition from chronic volatility to a more predictable digestive rhythm. While the search for a singular cure continues, this framework offers a sophisticated methodology for sustainable management.